Being a part of the Riverside County Public Health Department that covers Palm Springs, I have been involved in many discussions regarding the patient who died from Neisseria Meningitidis about 5 days after falling ill. He may have attended the White Party in Palm Springs on 3/30 and 3/31. He was ill on 4/8 and went to the Emergency Department on 4/10. The incubation period for this disease is 2-10 days. So if there was an outbreak we should have seen it by 4/10. We did not. It is now, as I write, 28 days after the White Party and we still don’t see an outbreak. This germ must be reported by any lab, hospital, or provider to the public health departments, so we know we are not missing these infections. Many of the labs have automated computerized reporting that doesn’t fail.
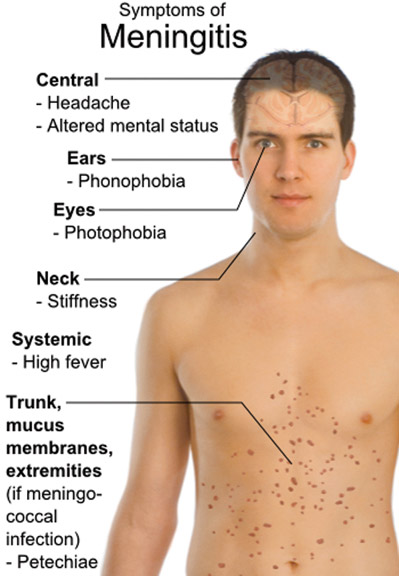 It is transmitted by close contact for weeks, as in a dormitory at college, or barracks of those in the armed services, therefore these are, as my son and nephew were, given the vaccine. It is also passed by kissing, not coughing. So it is not a “Gay” disease. There were many kisses at the White Party and still no outbreak is recorded.
It is transmitted by close contact for weeks, as in a dormitory at college, or barracks of those in the armed services, therefore these are, as my son and nephew were, given the vaccine. It is also passed by kissing, not coughing. So it is not a “Gay” disease. There were many kisses at the White Party and still no outbreak is recorded.
There is an outbreak in New York among gays because they are kissing, not because they are gay. The two gays who died in Southern California in December, 2012 do not constitute an outbreak since it stopped at 2 and there was no cluster, like in New York. This meningitis occurs here and there without an outbreak.
Our suggestion is to talk to your healthcare provider, especially if you have kissed a gay person from New York recently. Los Angeles, Riverside, and San Bernardino County public health departments have the vaccine for those who can’t afford it and are concerned. After explaining the facts to my patients, very few want the vaccine. The California State public health department and the CDC have been watching this situation closely also but do not feel it is time for calling it an outbreak, as in New York.
CIRCUMCISION
It has been found that bacteria that live in the foreskin can break down the skin barrier to HIV, allowing easier transmission across the skin barrier. This may explain why circumcision works to prevent HIV transmission. It is not 100% like abstinence or as good as condom use or the donor (bottom, HIV+) having an undetectable viral load, but it does help quite a bit. The British HIV Association has now officially stated that they recommend all patients with HIV have a discussion with their medical provider regarding treatment reducing transmission. In Africa where medications are less available, there are programs for circumcision.
VACCINE
This last year a great effort started to study new approaches to an HIV vaccine. I still have hope even though a recent vaccine study was stopped. Most large human studies have a Data Safety and Monitoring Board. The members are qualified to understand the research but are not involved in the study. They look at all the data once or more times before the end of a trial to make sure there are no scary side effects popping up or to see if the study isn’t going to prove the new treatment is better. In this study, as in others, they felt that continuing the study would not be helpful so they recommended terminating it. Why ask people to take a treatment when it is not going to work well? I think this is a great approach to limit risks to patients in studies.
AFRICANS MAY DIE AT HIGHER CD4 COUNTS
They found that the HIV negative person in a couple (discordant couple) was at higher risk of dying at lower the CD4 levels, as expected. This even was true for CD4s <500. They recommended that in Africa it may be better to start antivirals when at CD4 <500 which is earlier than they do now.
FATIGUE
Even though viral load is undetectable there is a good number of HIV+s who are fatigued. This may be associated with taking Zerit® or Videx® in the past.
VIRAMUNE® RESISTANCE
Viramune® and Efavirenz (in Atripla®, Sustiva®) are very prone to causing resistance if not given as triple therapy. A practice in the past was to give AZT or Viramune® to pregnant HIV+ mothers just before delivery, but many of these would have resistance develop, causing many problems later. Now they know that if they give triple therapy for 3 weeks, the chance of resistance is low. The other two medications protect the triple combination as a team. Don’t take some; take all or none every day.
RETENTION IN CLINIC
There is a progression from a person not knowing they are HIV positive, to being in care regularly for successful control and monitoring. It is important to move those who don’t know, to testing, and moving the positives to care and keeping them in care regularly. This takes skill and much effort on the clinic’s side to reach those who drop out at each stage along this progression. Patients should also do their part.
OKLAHOMA DENTIST MAY HAVE TRANSMITTED HEPATITIS C
A patient who had no other risk factors for Hepatitis C, came down with it. The health department inspected his dentist’s office and found equipment that wasn’t properly sterilized, needles and vials of medications that were reused so that infections from one may have been passed to another. About 7,000 patients are being notified to be tested for Hepatitis C, B and HIV.
Keep those questions coming. Be Safe!
Daniel Pearce, D.O., FACOI, AAHIVS
Associate Clinical Professor of Internal Medicine, Loma Linda University
HIV Specialist, Riverside County Public Health Department
Hepatitis C Specialist and Researcher, Southern California Liver Centers, Riverside
HIV Researcher, Desert AIDS Project
References: Medscape.com

